Modern Neurological Tools: Why the Pupilometer Is the Best?
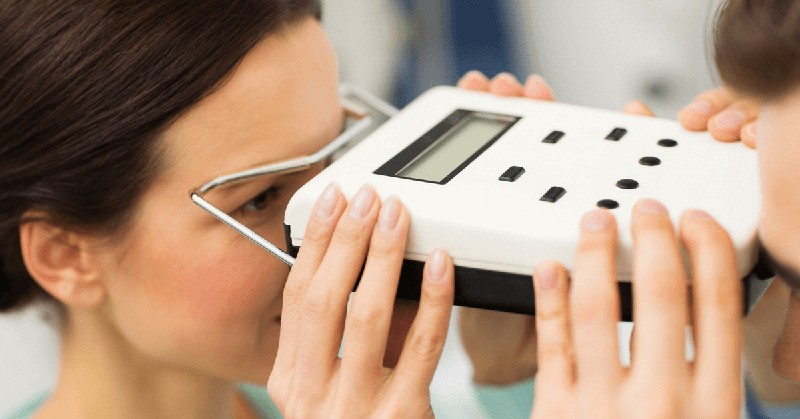
With traumatic brain injuries and other neurological issues, it’s difficult to diagnose precisely what is happening. Many conditions can affect the brain and cause a variety of symptoms and effects.
One tool used by doctors to help them determine what is going on in the brains of their patients is called a pupilometer. This device allows doctors to measure their patient’s pupil dilation velocity, giving clues as to what might happen inside their heads.
This device has proven effective at helping doctors diagnose the causes of various neurological issues, including brain trauma, strokes, and other medical problems.
This post discusses a pupilometer, how it works, and why doctors use it to diagnose patients.
What is a pupilometer?
A pupilometer is a piece of cutting-edge neurological equipment used to evaluate visual acuity and pupil reactivity.
The pupils provide improved nighttime vision by regulating the amount of light entering the eye. The optic nerve transmits images from the retina to the brain, and a doctor may check the health of the eye and the nerve by using a pupilometer. This is the test used by doctors when neurologic disorders are suspected.
How accurate is the pupillometer?
Because of the pupilometer’s ability to measure in real-time, it provides an accurate assessment of the size of the pupils.
The pupillometer requires just a quick eye scan and provides more reliable results than a manual evaluation would. Because of this, the patient and the doctor can complete the examination more quickly and with less effort. They aren’t at risk of damaging their eyes by undergoing risky manual exams.
Pupil Examination Is a Benchmark of Care and Is Important to Patient Outcome
One of the most critical diagnostic instruments in neurology and neurocritical care is pupillometry.
It provides a measure of the NPi and helps clinicians assess brain function and look for indicators of increasing intracranial pressure or herniation. Pupilometry is a standard diagnostic test in neurology and has helped predict recovery after TBI (TBI).
By measuring the degree to which the patient’s pupils dilate and constrict or “respond” to light, physicians may determine whether the patient is aware of their surroundings.
Manual Pupil Assessment is Highly Subjective and Inaccurate
Eye doctors used to rely on a physical pupil exam as the gold standard.
But it’s pretty open to interpretation and often wrong. Pupillary size, shape, sensitivity to light, and bilateral symmetry may all be evaluated with a manual evaluation performed by an ophthalmologist or nurse practitioner.
Pupilometry is a novel method of measuring pupil size faster for doctors and patients than traditional methods and is more accurate objective, and consistent.
The Use of Pupilometry in Neurocritical Care
TBI
Traumatic brain injuries result from a sudden, forceful, quick acceleration or deceleration of the head (TBIs).
Confusion, paralysis, loss of consciousness, and coma are only a few symptoms associated with traumatic brain injuries. Pupilometry is a non-invasive method that doctors may use to diagnose and treat traumatic brain injury. Pupil size is evaluated as a function of various light intensities.
Cerebral Edema and Increased ICP
An abnormal increase in brain fluid characterizes cerebral edema.
When the CSF fluid within a patient’s skull builds up to dangerous levels, this is called elevated intracranial pressure (ICP). Trauma, illness, and brain tumors are just a few medical conditions that might cause this symptom. Without treatment, high intraocular pressure (ICP) may cause irreversible damage to the eyes.
Pupilometry is used to gauge the severity of an eye problem by measuring how the size of the pupils varies.
Status Epilepticus (SE)
Treatment of status epilepticus (SE) must be prioritized as a medical emergency.
If neglected, it may cause irreversible brain damage or even death. When a seizure lasts over 5 minutes, or if there are many seizures with no complete return of consciousness in between them, SE is present. Pupillometry is useful in SE because it offers clinicians a sense of brainstem involvement, which aids in formulating a treatment strategy.
Ischemic and Hemorrhagic Stroke
When a brain blood vessel bursts, it may cause either an ischemic or a hemorrhagic stroke.
Ischemic strokes are caused by a clot that prevents blood from reaching the brain. If a blood vessel in the brain ruptures, it may cause hemorrhagic stroke, which damages the surrounding tissues. The pupil’s reaction to light will be distorted and asymmetrical after an ischemic stroke. Strokes caused by hemorrhage are often asymptomatic.