How Coverage Has Formed And Will Carry on To Shape Telehealth
Some will say 2020 was the 12 months that anything altered, but in truth, it will be 2021 that decides our new health care fact. Digital treatment innovative quickly—and under duress—last yr. How will we understand from the seismic shifts in care supply we knowledgeable many thanks to COVID-19? How can we aid providers and innovators embrace the transformation? How will we solidify these gains?
Dad’s Story: Telemedicine Pioneer
We think of telemedicine as a relatively the latest invention—only manufactured attainable by the net and good phones—but I had my 1st taste of it 60 several years in the past. As a medical doctor who was trained in the significance of putting your arms on a affected person to diagnose and heal—I have grow to be an ardent advocate for telemedicine following many years of observing it increase care.
My earliest experience was with my own health practitioner-father. When I was a youthful boy about 8 or 9 several years aged, the phone would ring in my parent’s bed room in the middle of the night three to four moments a 7 days. Dad was educated in what was then nevertheless the youthful specialty of cardiology. As just one of our region’s several cardiologists, providers in rural Tennessee relied on his knowledge. Every time the telephone would ring, Father would calmly communicate with a nurse or a health practitioner, and right after learning the patient’s signs or symptoms, would area the receiver on a clunky, antiquated gadget on his bedside desk that would read out the small blips of an EKG machine on a steady strip of paper. Father would seem at that EKG to make a prognosis and instruct a class of therapy. He was on the revolutionary front of utilizing telemedicine, applying distant technological know-how and monitoring, to link to sufferers all over the center third of the condition.
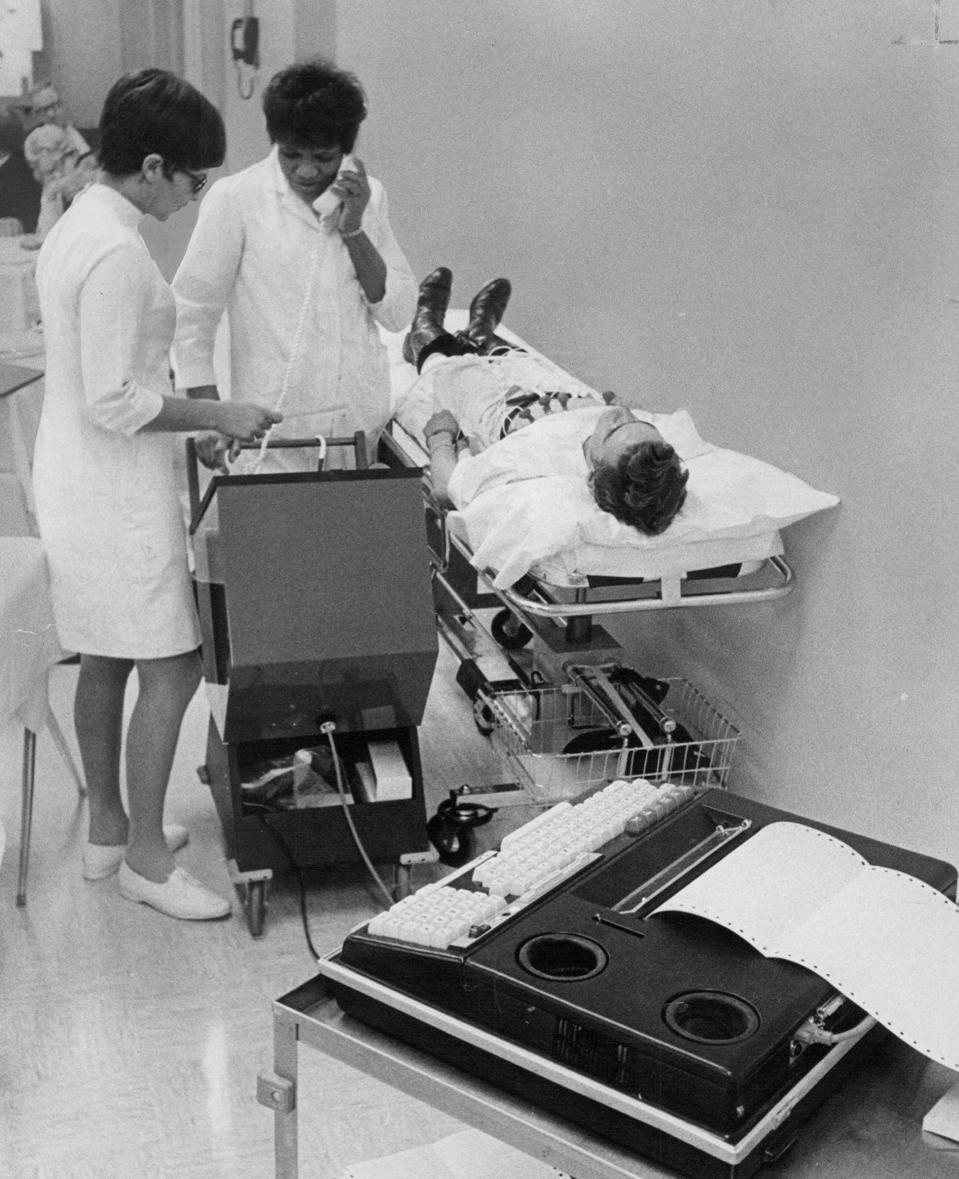
MAR 17 1971, MAR 18 1971 Mrs. Alleyene Menogan, Remaining, Oversees Automatic Cardio Evaluation Procedure … [+]
Decades later on in the 1980s, I relied on telemedicine in my personal apply as a coronary heart transplant surgeon to control the continual immunosuppressive treatment of my coronary heart recipients all over the place for months right after their transplants. And as the only health care provider in the Senate in the 1990s, I spearheaded big investments in courses developing costly T1 strains to Indigenous Americans on reservations which allowed us to give true-time telehealth to susceptible populations in remote regions.
Currently, as a lover and board member, I am intensely included with Teladoc Health and fitness, Livongo, and a digital dental care business, Smile Direct Club. In my 60-year journey with telemedicine, I have by no means been much more optimistic about our future as I am right now.
Recent Background And Modified Views
We are at an inflection level. The sheer scaling of telehealth solutions that took put across the nation above the program of the pandemic has been astounding. The explosion of digital treatment is the one most transformative—and most constructive—advancement to emerge from the COVID-19 crisis.
Vendors and health units have tirelessly stepped up to the challenge of adopting and proactively partaking patients in digital care:
- Pittsburgh’s UPMC observed movie visits, which were averaging 20-30 a day pre-pandemic, expand to 6,000 a day at the pandemic’s top.
- Kaiser Permanente—which now experienced a rather massive telehealth presence with about 15% of scheduled outpatient visits done virtually—saw that determine skyrocket to 80% in the early spring.
- The Centers for Medicare and Medicaid Expert services (CMS) shared that involving mid-March and mid-Oct about 24.5 million out of 63 million Medicare enrollees—more than a third—received a telemedicine provider.
- And we at Teladoc Health and fitness have found utilization stabilizing at a stage 40% better than prior to COVID.
Now, companies are scheduling and fiscally budgeting for a larger proportion of digital treatment, an approximated 10 – 30% of full affected individual visits post-COVID.
This is a seismic shift in the culture of telehealth. The culture of doubt, of fears around privacy, of insufficient reimbursement, of the unknown, was changed by a tradition of assurance and have confidence in, a society which values convenience, affordability, and fast access to high-quality care. All this in the protected ecosystem of household, removing the danger of COVID spread.
With this adjust, companies are progressively relaxed conducting virtual visits and are seeing the advantages. A latest American Professional medical Association survey of almost 1,600 doctors and other well being specialists identified that 60% described that telehealth has enhanced the overall health of their clients and 80% indicated it had improved the timeliness of care.
Equally, Americans are ever more at ease with virtual visits, with a single latest HIMSS study displaying 77% of people willing to use some form of telehealth publish-COVID, and 41% preferring it.

Shut up of a father with his son consulting with their medical doctor more than a movie connect with on the notebook
This cultural acceptance is currently significantly boosting mental and behavioral health access, significantly strengthening client convenience and knowledge, expanding individual adherence, and expanding achieve to areas with provider shortages.
How, then, do we protect and expand the gains produced when this general public wellness emergency will come to an finish?
How Coverage Has Shaped and Will Go on to Condition Virtual Treatment
We have to realize that the swift development was made doable by crisis regulatory actions that speeded access and reimbursement for telehealth solutions, producing physician adoption possible, and eradicating conventional bottlenecks in administrative decision-making.
Medicare supplied payment parity and waived geographic limits. Medicaid expanded protection, including protection of audio-only treatment.
CMS extra 144 further companies that could be furnished via telehealth and calm physician interstate licensure, waiving Medicare and Medicaid’s specifications that practitioners be certified in the condition where they are providing companies. And HIPAA information privateness guidelines were being peaceful, permitting companies to use non-HIPAA compliant telehealth platforms, like FaceTime and Skype.
Importantly, personal insurers followed the federal government’s direct, waiving charge-sharing and increasing telemedicine packages.
The Centers for Medicare and Medicaid Expert services, the Administration, and the non-public sector need to be commended for responding so promptly and so comprehensively to meet the rapidly switching requires of our healthcare communities through the pandemic.
But now we ought to make these gains long term.
Many of my previous Congressional colleagues—Democrat and Republican—are in favor of undertaking just that. Some required policies were being included in the year-end paying out and COVID-19 reduction bundle. Funding was amplified for the Federal Communications Commission’s telehealth work and expansion of broadband, and Medicare expanded protection for telemental overall health companies.
But I concur with American Telemedicine Affiliation President Ann Mond Johnson: “The recognizable deficiency of permanent reform or a assured extension of the telehealth flexibilities in this relief offer is disheartening for the millions of Americans who relied on telehealth to obtain treatment, and our health care providers even now on the frontlines of the pandemic. We consider arbitrary limits on telehealth need to be forever taken out to make way for a modernized and a lot more obtainable health care program.”
I served 9 months in an equally split, 50 to 50, Senate. With a razor-slim Democratic bulk in the Senate that is issue to filibuster, I’m regularly asked where by we might see bipartisan arrangement in health coverage in 2021. Telehealth is unquestionably at the major of that record.
To continue on this development, we need to forever make it possible for telehealth entry irrespective of affected person and provider site and codify the broader selection of practitioners including bodily therapists, occupational therapists, and speech language pathologists to present Medicare telehealth companies. Congress must also address cross-condition licensing limitations, even though this will be a extra challenging spot to navigate.
Federally Skilled Health Facilities and Rural Health Clinics—community-centered health treatment suppliers that support underserved populations—should be authorized to keep on to present telehealth right after COVID and reimburse all varieties of communication similarly if suppliers can satisfy the same benchmarks of care.
Whilst the Administration has finished a fantastic occupation, there is a danger that wide telehealth deployment—if not very carefully designed—could replicate the barriers of the standard bricks and mortar wellness process that generate disparities.
One obtrusive example is a bias in some of the new authorizations for two-way video communications. If we discriminate against phone (without having online video) consumers, for example, we will depart behind rural communities with no access to broadband, as properly as minority and other lower-cash flow populations that might not have more high-priced good telephones with two-way movie capabilities.
Eventually, when I think most regulatory alterations manufactured to progress telehealth and digital care during these incredible occasions must be produced long lasting, parity in payment is a single that really should be revisited adhering to the disaster. Without doubt, payment parity was vital to motivate health practitioner participation. But due to the fact several overhead expenses are eliminated in virtual transactions and consequently outcome in overall charge personal savings, these savings really should stream to the individual as nicely as the company.
To reiterate, we are at an inflection point. And inflections bring new worries, and inflections desire altered perspectives—changed comprehension, and adjusted behaviors on our pieces. We have the opportunity to embrace these variations and unleash an exciting new frontier of digital care, with the public sector reimagining regulatory pointers to allow for private sector innovation to increase to satisfy individual desire and improve treatment for all.
This op-ed is primarily based on remarks I sent on January 12, 2021 at the American Telemedicine Affiliation EDGE Plan Meeting. A movie of the whole remarks is accessible on the net.